Having two different chronic illnesses of any kind can be difficult to manage. And there appears to a prevalence of type 1 diabetes and celiac disease. These are two autoimmune disorders that can be problematic for an individual’s health. So, in this article, we are going to discuss the comorbidity of diabetes and celiac disease. Before getting into the details, here’s a brief summary.
Diabetes and Celiac Disease: There appears to be about an 8% prevalence of celiac disease among patients with type 1 diabetes. There may be overlapping factors between diabetes and celiac disease, such as genetic and environmental factors. The comorbidity of these disorders can make treating one or the other more difficult. Here is what you need to know about diabetes and celiac disease.
What is Celiac Disease?
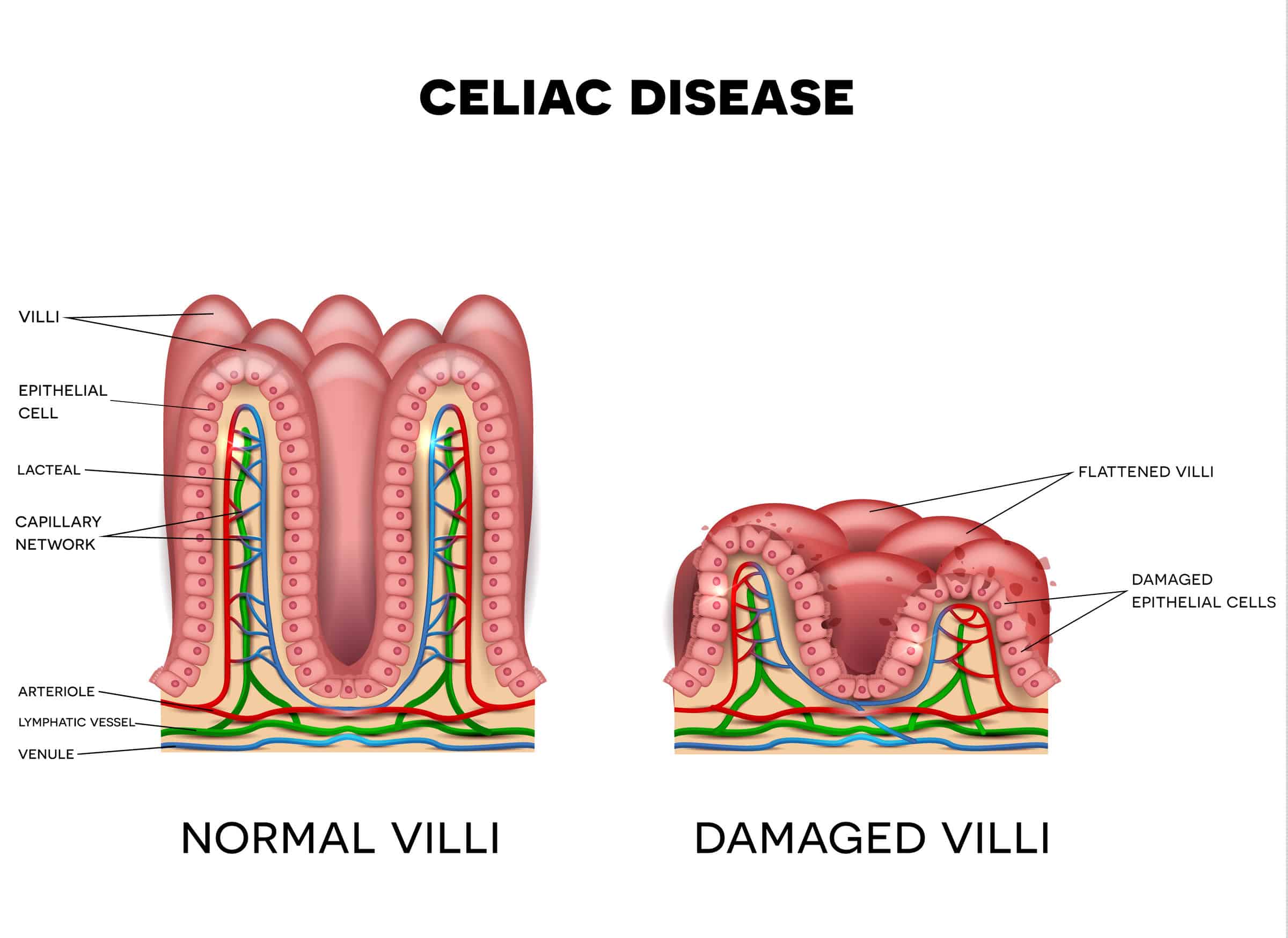
Celiac disease is an autoimmune disorder that causes an individual to have sensitivity to gluten. So, a person with this condition will experience an immune response in your small intestines caused by gluten. The small intestines is lined with villi. These villi are responsible for absorbing vitamins, minerals, and other nutrients from the food you eat. When you have celiac disease, though, the villi become damaged and flattened. Thus, your small intestines is not able to absorb enough nutrients.
The gluten sensitivity caused by celiac disease can cause serious complications long-term. This is because one’s reaction to gluten can cause damage to the lining of the small intestines. Ultimately, this can lead to diarrhea, fatigue, weight loss, bloating, and anemia. 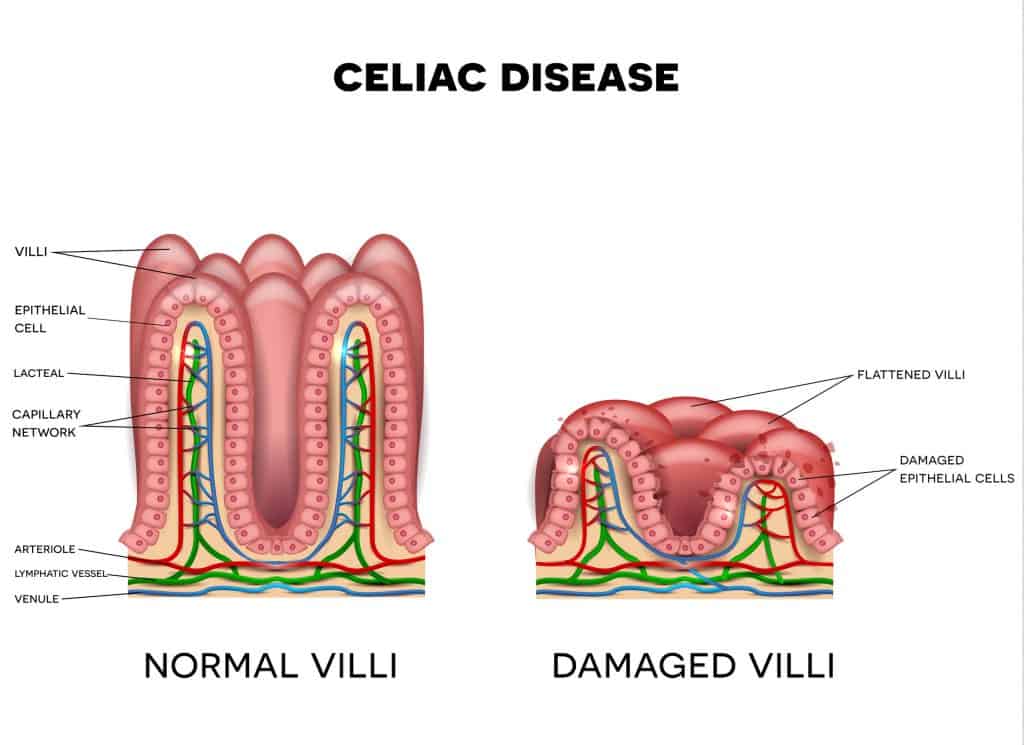 Symptoms of celiac disease may vary from individual to individual, but they may include:
Symptoms of celiac disease may vary from individual to individual, but they may include:
- Diarrhea
- Fatigue
- Weight loss
- Bloating or gas
- Constipation
- Abdominal pain
- Nausea
- Vomiting
- Osteoporosis or softening of the bones
- Mouth ulcers
- Joint pain
- Skin rash
- Headaches
There are a variety of complications associated with celiac disease. One of these complications may include malnutrition. Malnutrition occurs when the small intestines cannot absorb enough nutrients, which can lead to weight loss and anemia. Other complications include increased risk of cancer, miscarriage, infertility, weakening of the bones, lactose intolerance, and nervous system problems.
Is there a Link Between Diabetes and Celiac Disease?
Celiac disease is more prevalent among type 1 diabetes patients when compared to the general population. Genetic and environmental factors may play a role in the link between diabetes and celiac disease.
It is important to note that there is no link between type 2 diabetes and celiac disease.
Both type 1 diabetes and celiac disease are considered immune-mediated conditions, and there is about a 6-8% overlap among patients. The major link between diabetes and celiac disease is their similar genetic traits. This means that both of these autoimmune disorders can be triggered by similar factors, causing the body’s immune system to attack itself and destroy healthy tissue.  Now, the exact cause of either type 1 diabetes or celiac disease is not very clear. It is clear that consuming gluten will trigger symptoms of celiac disease, but that may not be what causes it.
Now, the exact cause of either type 1 diabetes or celiac disease is not very clear. It is clear that consuming gluten will trigger symptoms of celiac disease, but that may not be what causes it.
People can consume gluten products for years without any small intestinal problems. The same goes for type 1 diabetes. Doctors know how to diagnose and treat the condition, but the cause of it is not clear. Family medical history is believed to put a person at an increased risk. However, there a many individuals that end up with a type 1 diabetes diagnosis that have no family history of this disease.
Ultimately, the overlapping characteristics in the genes of diabetes and celiac disease is the link. What exactly this means for causation of comorbidity, is that the thing that causes celiac disease may also be the cause of type 1 diabetes, and vice versa.
Diagnosing Celiac Disease in Diabetes Patients
Because there has been a prevalence and link between celiac disease and diabetes, those that have type 1 diabetes are recommended to be screened regularly. Diabetes patients need to be screened regularly because the beginning symptoms of celiac disease can often be subtle and overlooked. Patients with celiac disease may be asymptomatic in the beginning stages, making it difficult to diagnosis early on.
Therefore, two tests can help physicians screen patients for celiac disease. One test is a serology test. A serology test is a blood test that looks for antibodies in your blood to identify if you have been exposed to a certain infection. So, if specific antibody proteins are found in your blood, then that may indicate that your immune system has a reaction to gluten.
A genetic test is one that looks to identify specific genes in patients. Patients that carry one or both of HLA DQ2 and DQ8 may have an increased risk of developing celiac disease.
It is important to note that you should be tested before eliminating gluten from your diet. Going gluten-free prior to being tested may cause the test to return normal, and you may be misdiagnosed. If either of your tests come back positive, then your doctor may order more screening to be done. This may include either an endoscopy or a capsule endoscopy. This allows the doctor to view the small intestines.
Does Celiac Disease Affect Blood Sugars
Celiac disease can certainly affect blood sugar levels if you have diabetes. Those with celiac disease may experience malabsorption of nutrients that can lead to low or high blood sugar levels. The majority of the time, patients experience low blood sugar levels since the small intestines is not able to absorb carbohydrates as well. Having type 1 diabetes and celiac disease can lead to uncontrolled blood sugar readings and a higher A1c. This can lead to more health complications if left untreated.
Managing Diabetes and Celiac Disease
Managing diabetes and celiac disease can be difficult, but it is not impossible. You have to determine what you can and cannot eat, then learn to adjust your dose of insulin based on your food consumption.  So, to treat gluten-sensitivity, you have to do your best to avoid gluten. Foods that contain large amounts of gluten include:
So, to treat gluten-sensitivity, you have to do your best to avoid gluten. Foods that contain large amounts of gluten include:
- Pastas
- Noodles
- Breads
- Crackers
- Baked goods and pastries
- Granola
- Cereal
- Breakfast foods (French toast, pancakes, waffles, etc.)
- Sauces and gravy
- Breading and other mixes
It is important that when getting certain foods that you check the label. Many foods that seem like they would contain gluten have different ingredients and are labeled “gluten-free.”
By going gluten-free, you can avoid any pain and damage in the small intestines caused by celiac disease. It may be difficult to gain control over your blood sugar readings after going gluten-free.
As mentioned above, many patients with diabetes and celiac disease experience hypoglycemia before going gluten-free. So, after making adjustments to your diet, you may experience blood sugar readings that are higher and more difficult to manage. This is because the small intestines will be able to heal and absorb more carbohydrates than before. Consuming carbohydrates that are higher in fiber may prove to help you prevent hyperglycemia.
The most important advice we can give is to talk to your doctor about your condition. Your doctor will be able to make accurate suggestions for adjusting your insulin doses.
Conclusion
We hope this has given you greater insight into the connection between diabetes and celiac disease, as well as how you can better manage the combination of these illnesses. We, as much as anyone, understand that affording medications you need is difficult and makes managing your health condition even harder. Prescription Hope is able to provide access to medications for individuals at the set cost of $70.00 a month through Prescription Hope’s medication access service for each medication. We work directly with pharmaceutical manufacturers and utilize their patient assistance programs on behalf of our patients. For those who do not qualify, we find other ways to save. Whether substitute meds and their programs, or discount cards and coupons – our staff works hard to help you save on your monthly medication costs.
Enroll with us to find out if you are eligible and start saving money.