A continuous glucose monitor (CGM) may also be called a glucose sensor. A glucose sensor can prove to be beneficial for those looking to lower their A1c and gain better control over their blood sugar levels. However, understanding how a glucose sensor works will give us a better understanding of how to use them properly. So, in this article, we’ll discuss how glucose sensors work, why their beneficial, and who they are for. Here is a quick summary for you before getting into more detail.
How Does a Glucose Sensor Work? A continuous glucose monitor or sensor is a small device that attaches to the body and gives a continuous reading of blood sugar levels. It measures the level of glucose in the interstitial fluid. The sensor transmits the readings to a smartphone or another device. Here is everything you need to know about how glucose sensors work.
Different Types of CGMs
There are three main glucose sensors on the market currently. They are the Freestyle Libre, Medtronic’s Guardian 3, and the Dexcom G6. Those are the most up to date models at the time of writing, though other models may exist currently. Other companies may also be developing models in the near future as well.
The Freestyle Libre may be the simplest one to use. It is about the size of two quarters stacked together and is placed on the back of the arm. You can scan the sensor with the reader or the Freestyle app on your smartphone. Both the Dexcom and Medtronic glucose sensors are very similar. The sensor for these brands are placed on either the abdomen or back of the arm. After the sensor is applied, a small transmitter is attached. The transmitter sends the glucose reading from the sensor to the individual’s smartphone or another device.
Overview of How Glucose Sensors Work
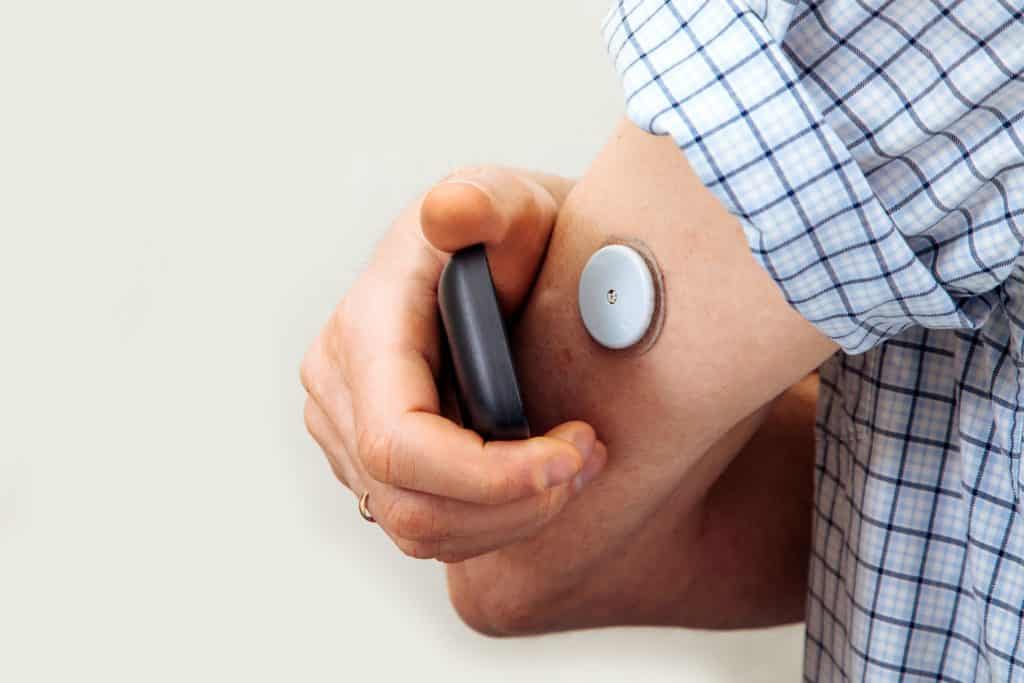 Regardless of the type of CGM you get, they will each come with an applicator that allows you to insert the sensor easily. The applicator uses a loaded spring to insert the sensor. The tiny sensor is a flexible filament that sits just under your skin and is attached to an adhesive above the skin. After the glucose sensor is applied, it will require a warm-up period. The length of the warm-up period is typically 1-2 hours. There will be no glucose readings from the sensor during this time. It is needed so that the sensor can acclimate to the body. The sensor continuously measures glucose and sends the reading to a display device wirelessly every five minutes.
Regardless of the type of CGM you get, they will each come with an applicator that allows you to insert the sensor easily. The applicator uses a loaded spring to insert the sensor. The tiny sensor is a flexible filament that sits just under your skin and is attached to an adhesive above the skin. After the glucose sensor is applied, it will require a warm-up period. The length of the warm-up period is typically 1-2 hours. There will be no glucose readings from the sensor during this time. It is needed so that the sensor can acclimate to the body. The sensor continuously measures glucose and sends the reading to a display device wirelessly every five minutes.
The glucose sensor works regardless of what you are doing whether that be showering, sleeping, or exercising.
Some glucose sensors will even send alerts to your device to notify you of high or low blood sugar levels. This can be lifesaving in some circumstances. A person with diabetes that struggles to wake up from low blood sugar in the middle of the night will find this extremely beneficial. This can also help individuals prevent rapid fluctuations in blood sugar levels.
Be aware that certain glucose sensors may require calibration every 12 hours. Calibrating the sensor means manually checking your blood sugar by pricking your finger and testing the glucose on a blood glucose meter. You then enter the reading from the manual test into the sensor platform. This allows the sensor to calibrate and ensure an accurate reading.
Some sensors need calibration because the sensor doesn’t actually measure the blood glucose. It measures the glucose level of the interstitial fluid. New developments are being made with glucose sensors allowing some of them to work directly with insulin pumps. This creates a closed-loop insulin delivery system, which is also known as an artificial pancreas.
Difference Between Glucose Sensors and Blood Glucose Meter
Measuring your blood sugar level through a finger stick and a blood glucose meter will provide you with the most accurate reading of your blood sugar level. This is because it measures the glucose in the blood.
A glucose sensor works by measuring the glucose level of the interstitial fluid. This is the thin layer of fluid surrounding the cells. Therefore, the glucose sensor reading may be slightly delayed when compared to the true blood glucose reading. The variation will be greater if a person’s blood glucose is in rapidly rising or declining. This happens shortly after eating or administering insulin.
If blood sugar levels are stable, then there will be less variation between the two readings. Typically, the glucose sensor reading will experience about a 10-minute delay when compared to a blood glucose meter. So, it is still crucial for a diabetes patient to keep a blood glucose meter and test strips on them. If there is any doubt in the accuracy of the glucose sensor reading, then manually check your blood sugar with a glucose meter.
Who Should Use a CGM?
 Those with type 1 diabetes will benefit the most from using a glucose sensor. However, people with type 2 diabetes may also benefit from wearing a CGM also.
Those with type 1 diabetes will benefit the most from using a glucose sensor. However, people with type 2 diabetes may also benefit from wearing a CGM also.
Thankfully, glucose sensors are approved for both adults and children to use. Even children as young as two years old may be approved to use certain glucose sensors.
Your doctor may suggest that you use a glucose sensor if you are on intensive insulin therapy, have hypoglycemia unawareness or uncontrolled blood sugar levels.
A glucose sensor can help you gain better control over your blood sugar and diabetes condition, as it provides you with trends in your blood sugar readings, and you can see what exactly is affecting the levels. If you have low blood sugar levels often, then using a CGM can help you prevent your glucose from getting too low. It gives you an opportunity to treat it before it becomes a problem. You may also want to use a glucose sensor if you have to prick your finger many times a day. The glucose sensor can lower the number of finger sticks you are performing each day.
How Long do Glucose Sensor’s Last?
The length of time each sensor lasts will vary slightly depending on the brand.
- The Freestyle Libre will last 14 days.
- The Dexcom G6 will last up to 10 days.
- The Medtronic Guardian 3 will last up to 7 days.
It is important to note that the glucose sensors attach to the body through an adhesive. If the adhesive wears out from body sweat or something else, then the sensor may not last the full length of time. There is also a chance of the sensor getting caught on something causing it to get ripped off. Once the sensor comes off, you cannot put it back on. A new sensor will be needed to replace it.
The Cost of CGM
The cost of glucose sensors will also vary from brand to brand and will also depend on an individual’s insurance. Here is the approximate cost of the most popular glucose sensors for cash-paying customers.
- The out-of-pocket cost for the Freestyle Libre starter kit is about $215. The starter kit consists of the reader and two 14-day sensors. Each 14-day sensor cost about $67.
- The out-of-pocket cost for the Dexcom G6 is about $349 for 3 10-day sensors. The transmitter will cost between $145-236. If the patient needs a receiver, then it will be about $365 from Dexcom.
- The out-of-pocket cost for the Medtronic Guardian 3 transmitter is about $700. Each 7-day sensor will cost between $70.00-$75.
It is important to note that the transmitters usually last a long time, as long as the individual takes care of it. The Freestyle Libre does not require a transmitter. All of the glucose sensors have free apps available for your smartphone.
Conclusion
Glucose sensors can be complex devices. So, we hope this has given you a better understanding of how glucose sensors work and the cost of them. Overall, this device can help individuals with diabetes lower their A1c and gain better control over their condition.
Prescription Hope is a nationally recognized pharmaceutical access service program that helps individuals access affordable medication. We work with 180 pharmaceutical manufacturers and their patient assistance programs to provide individuals with access to their medication at the set, affordable cost of $70.00 a month through Prescription Hope’s medication access service for each drug. If a patient does not qualify, we still look to help them save. From manufacturer coupons to discount cards, we work to help you find a solution to your high medication costs.
Enroll with us to see if you are eligible and let us help you save money every month.
